As I first outlined here in a post from 2018, our Chair of Logistics Management applies scientific methods to ensure the arrival of critical supplies at the right place, at the right time, and at the lowest cost. This goal sounds deceptively simple, but faces challenges that increase dramatically as the available resources and infrastructure diminish. This usually happens in a humanitarian context. The pandemic reinforced the urgency of well-designed logistics as reports of shortages of Personal Protective Equipment (PPE) hit the news. The thought of a doctor without mask or gloves treating a contagious patient is intolerable, and motivates our work on logistics preparedness in Uganda.
- Home
- Blog
- Development & Sustainability
- Humanitarian Logistics: Epidemic Response in Uganda
Humanitarian Logistics: Epidemic Response in Uganda
by Bublu Thakur-Weigold, Chair of Logistics Management MTEC, ETH Zurich, 16 December 2021

Photo credit: iStock
ETH’s HumOSCM lab supports logistics preparedness for disease outbreaks in Uganda. In the midst of the global pandemic, this project with Uganda’s Ministry of Health is more important than ever.
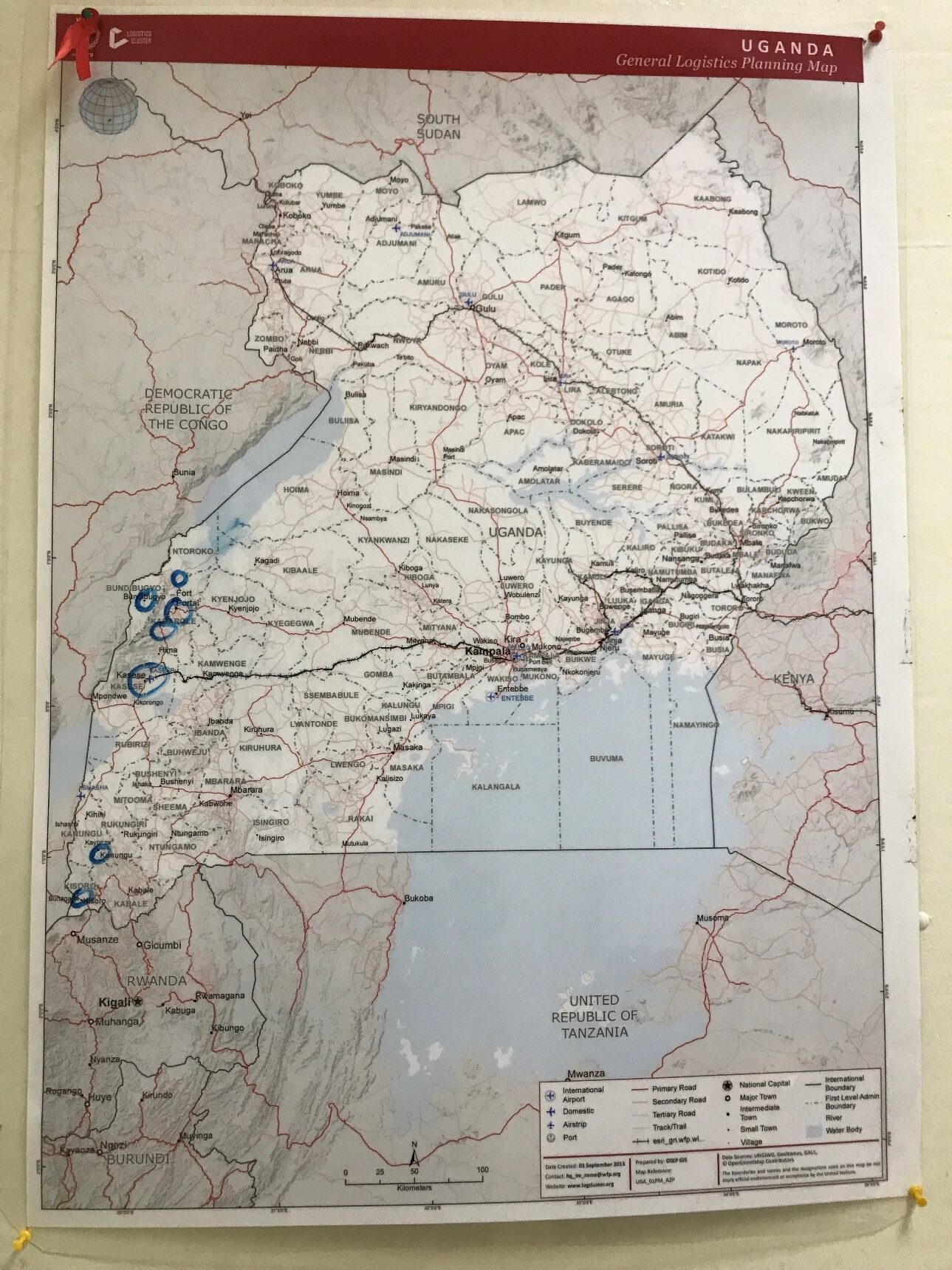
Photo credit: Bublu Thakur-Weigold
Even before the spread of the Covid-19 virus, Uganda routinely faced heightened risks to public health from epidemic outbreaks. A number of conditions - including a landlocked geographic location, the proximity of human settlements to animal populations, the migratory patterns of birds, and borders with “bad neighbors” like war-torn South Sudan - converge to produce pathogens which are often zoonotic (transmitted from animals to humans). The country which tourists fondly refer to as the “Pearl of Africa”, is therefore regularly confronted with outbreaks of diseases like Cholera, Marburg virus, West Nile fever, Malaria, and Ebola, with Covid-19 simply the latest addition to the list. Should its authorities fail to contain an outbreak, a population of 45 million inhabitants are directly at risk, and Covid-19’s variants have shown how quickly local outbreaks can threaten the global population.
ETH’s collaboration with the Ugandan Ministry of Health began with a workshop on the Ebola response in 2020. As we packed up to leave Kampala, the participants mentioned that a disturbing new pulmonary disease had been reported.

Photo credit: Bublu Thakur-Weigold
Research shows that the logistics operations consume up to 60% of the healthcare budget, mostly because of the supply costs. In a race against time, a well-designed logistics system not only enables the availability of life-saving medical equipment, the efficient use of scarce resources uses the healthcare budget to treat more patients.
ETH’s HumOSCM lab first visited Uganda in 2020 to work with the multiple humanitarian organizations who had responded to the Ebola outbreak in its Kasese province. Since then, working closely with the Ministry of Health revealed extensive medical experience with disease treatment and control. There was, however, a knowledge gap in the structure of the healthcare system. Because doctors and pharmacists are not trained in logistics, the design of the supply chain is usually an afterthought, with fateful consequences. A Ugandan army officer whose unit had supported the emergency medical transport, compared the disease response to war: “The field commander may have very beautiful combat strategies, but if his logistics commander is not up to the tasks, [the enemy] would kill them all…. because everything requires logistics and you cannot tell HR to do logistics, you cannot tell someone from the lab to do logistics.” To their credit, the leadership of the Ministry of Health recognized the importance of logistics from their experience of past outbreaks, and was ready to build capacity.
The emergency response to the Ebola outbreak in Kasese province involved over a dozen international organizations, whose complex logistics were led by the World Food Program.
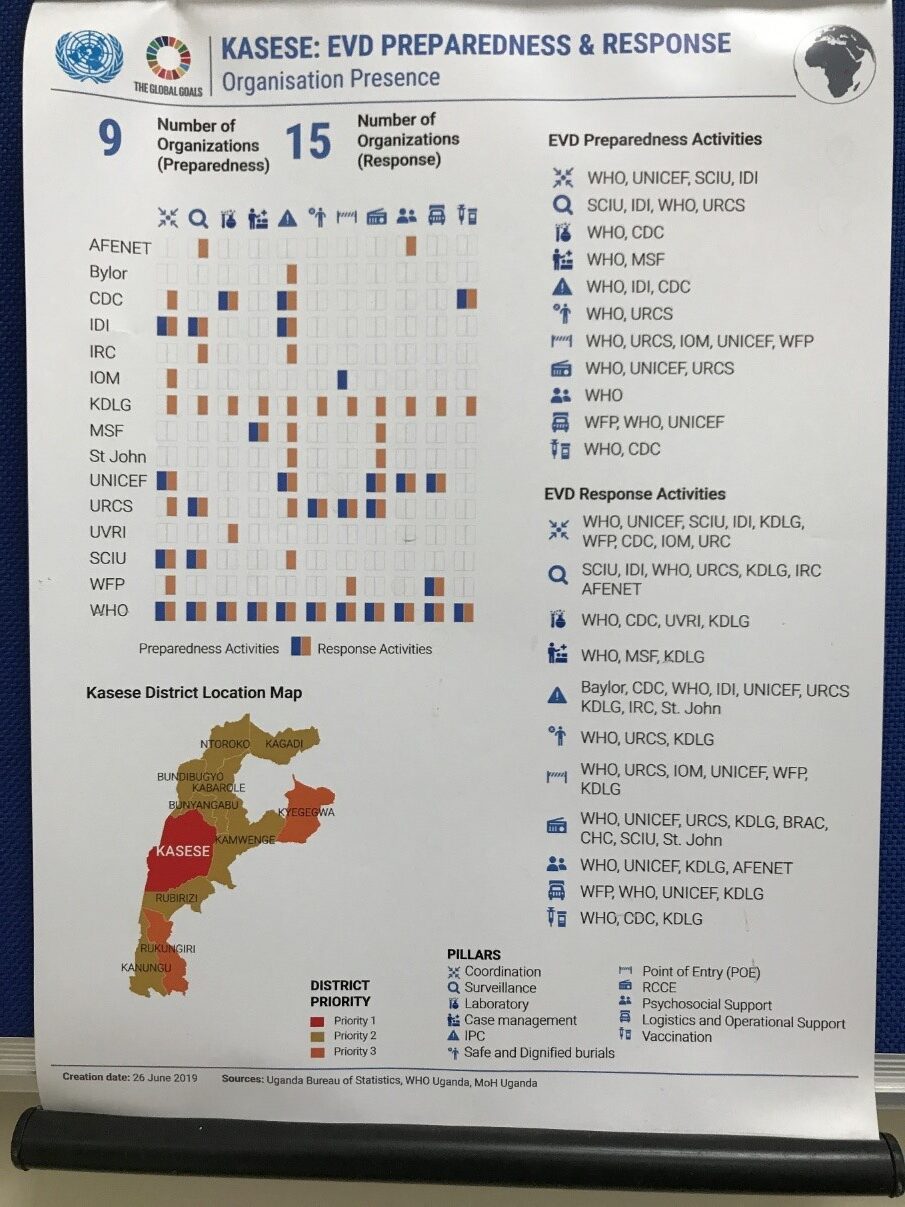
Photo credit: Bublu Thakur-Weigold
The project team has had its share of “Aha!” moments and unexpected insights. For example, Switzerland’s own emergency response to Covid-19 showed how much developed nations can learn from Uganda. When Eliane Müller’s master thesis benchmarked international protocols, she uncovered a lack of standard forecasting methods for disease outbreaks. The international CDCs, to which Uganda looked to for guidance, themselves expressed an interest in how we design the planning process. Local data confirmed that the responsiveness of Uganda’s regular healthcare supply chain, with its efficient and reliable replenishment processes, does not (cannot logically), fit the needs of an emergency response. The Ministry of Health acknowledged that supply chain segmentation with a portfolio of responses would be necessary, and posted our baseline assessment on its website (link below). Doctoral researcher Laura Heuser is rigorously modeling how much, and where, to pre-position medical supplies in an expansive terrain, so health workers don’t have to scramble. The project is currently summarizing the findings of dozens of focus groups. These were conducted online, with some respondents in remote regions dialing in from their cars to ensure power for the internet.
Pending travel restrictions, we will test prototype solutions in the field in 2022. We are eager to see the results, but not just for the sake of our friends and colleagues in Uganda. The global Covid-19 pandemic has made all of us potential beneficiaries of better-designed emergency disease response.

Photo credit: Bublu Thakur-Weigold
References
The project is supported by an ETH4D Research Challenges Grant financed by the Swiss Agency for Development and Cooperation (SDC).
Bublu’s 2018 post on humanitarian logistics
Link to the Ugandan Ministry of Health’s document library with the ETH report
ETH HumOSCM lab at MTEC’s Chair of Logistics Management

Photo credit: Bublu Thakur-Weigold
About the author
Bublu Thakur-Weigold is Associate Director Programs of the HumOSCM Lab at ETH Zurich's Chair of Logistics Management where she works with international humanitarian organizations to improve performance using scientific knowledge and research findings. She trained as an industrial engineer, and gathered over 20 years of supply chain experience in industry and consulting before joining the ETH as a researcher, lecturer, and program director.


